|
Concurrently, the use of IM nail fixation for distal tibia fractures has increased in popularity in the past 2 decades. The relative indications for IM nailing have expanded to include more distal fractures as modern implants have evolved to include more multiplanar locking options. Rate of fracture union and time to union are similar between the two treatment types and appears to be more affected by other patient and injuries factors, such as smoking, degree of soft tissue damage and open fracture. IM nailing provides a more minimally invasive approach compared with traditional open reduction with locking plate fixation, while respecting the soft tissue of the distal leg and allowing for early weight-bearing and return to function. Discussionĭistal-third tibia fractures (Orthopaedic Trauma Association classification type 43A) are challenging injuries to treat. Full-length AP (a) and lateral (b) radiographs demonstrate anatomic reduction of the fracture and correction of the varus malalignment at the fracture site. Three distal interlocking screws were placed, including one in the A-P trajectory, as shown (d). Anatomic alignment was confirmed on biplanar fluoroscopy as shown (c). This new lateral cortex forces the nail out of the malaligned path (b). Two A-P blocking screws were placed in the lateral aspect of the distal fracture fragment, creating a new lateral cortex in the metaphyseal bone. After removal of the interlocking screws, the nail was backslapped to the level of the fracture (a). The patient was made weight-bearing as tolerated in the postoperative setting (Figure 5). Lastly, two proximal interlocking screws were placed. Three distal interlocking screws were placed, including one in the A-P trajectory (Figure 4). Anatomic alignment was confirmed on biplanar fluoroscopy. The nail was passed down into the distal fragment with the block screws creating a new lateral cortex in the metaphyseal bone. 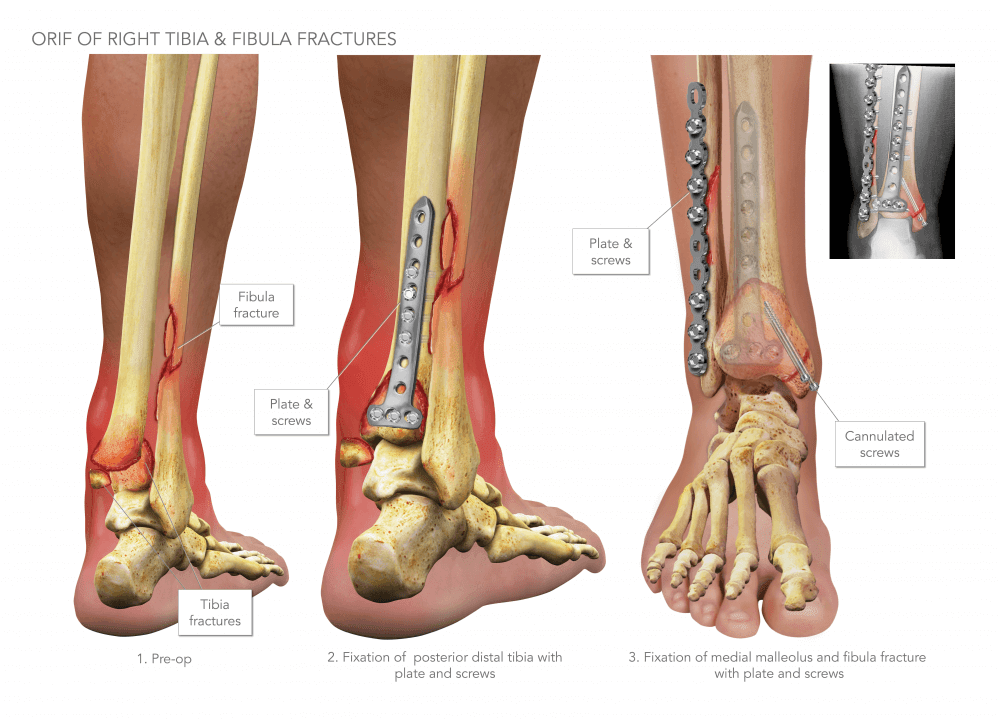
Two blocking screws were placed in an anterior-to-posterior (A-P) trajectory in the lateral aspect of the distal tibia to force the nail out of the malaligned path. The fracture site was found to be mobile and was reduced via closed methods. The distal interlocking screws were removed, and the nail was backslapped to the level of the fracture. After removing the interlocking screws proximally, the nail insertion jig was threaded to the proximal end of the nail. Revision IM nailing with blocking screw placementįor the revision surgery, an infrapatellar approach was used. What is the best next step in management of this patient? AP (a) and lateral (b) radiographs from the patient’s 6-week follow-up visit demonstrated varus collapse at the fracture site with no interval callus formation, demonstrating the windshield wiper effect on the short distal fragment. She elected to undergo revision IMN to correct the varus deformity. Her radiographs demonstrated varus collapse at the fracture site (Figure 3). Her wounds demonstrated appropriate healing without concerning features of underlying infection. Six weeks after the index procedure, she presented for routine follow-up and reported persistent pain at the fracture site exacerbated by weight-bearing. An orthogonal screw was not placed in the distal fragment. Two proximal and two distal interlocking screws were then placed. Anatomic reduction of the fracture was achieved as evidenced on postoperative full-length AP (a) and lateral (b) radiographs. She was made weight-bearing as tolerated and discharged after an uneventful postoperative course. The patient underwent debridement of the open fracture with intramedullary (IM) nail in the semi-extended position (suprapatellar IMN) (Figure 2). AP (a) and lateral (b) radiographs demonstrate a right distal-third tibia and fibula fractures with a medial open wound. Preoperative CT of the ankle did not reveal intra-articular extension into the tibial plafond. The wound was open medially approximately 2 cm with minimal contamination.  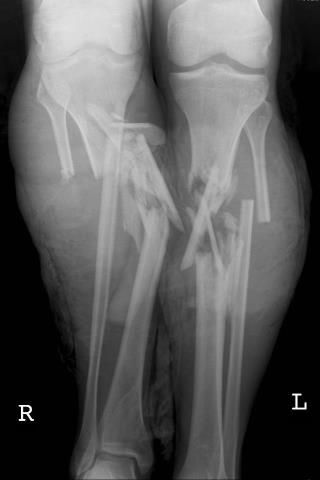
The patient was neurovascularly intact with soft compartments. The patient was appropriately resuscitated, given IV antibiotics, tetanus booster and cleared for surgery by the general surgery trauma team. If you continue to have this issue please contact to HealioĪ 42-year-old woman was involved in a motorcycle crash and sustained a type II open, right distal-third tibia and fibula fractures (Figure 1).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
